Understanding HPV: Most Common Sexually Transmitted Infection
11 January, 2023



The Human Papillomavirus (HPV) is a common virus typically spread through sexual contact. Some HPV infections may self-resolve without any symptoms. However, several subtypes may lead to chronic, persistent infections that put one at a higher risk for certain cancers.
What is Human Papillomavirus (HPV)?
HPV is a common virus that can affect different body parts, affecting both men and women. It is transmitted through sexual contact, including oral sex or close skin-to-skin genital contact with an infected individual. It can be passed even when an infected person has no signs or symptoms. HPV, which affects the genitals, is a Sexually Transmitted Infection (STI).
STIs fall into two groups:
- Low-risk: Usually asymptomatic, but some may cause warts on or around the genitals, anus, mouth or throat.
- High-risk: may cause several types of cancer.
How is HPV related to cervical cancer?

Certain strains of HPV (most often types 16 and 18) can cause changes in the cells of your cervix, a condition called Cervical Dysplasia. Your cervix is the opening between your vagina and your uterus. Left untreated, cervical dysplasia sometimes advances to cervical cancer.
Symptoms of HPV
Low-risk HPV does not typically cause symptoms, and as a result, most people are unaware of an infection. The body’s immune system may clear the infection in a few years. In some people, low-risk HPV can cause different kinds of warts, depending on the virus type:
- Genital warts: Either flat spots or raised bumps. In women, they usually grow on the vulva but can also appear on the anus, cervix or vagina. Men get them on the penis, scrotum or anus.
- Common warts: <span”><span”>Rough bumps typically appear on the hands and fingers.
- Plantar warts: Hard, grainy, painful bumps affecting the bottom of the feet.
- Flat warts: Slightly raised spots with a flat top that can appear anywhere on the body, most commonly on the face and legs.
Factors that put you at risk for contracting HPV:
- Several sexual partners: Having multiple sexual partners increases a person’s risk of contracting a genital HPV infection. Engaging in sexual activity with a partner who has had numerous sexual partners also puts a person at higher risk of contracting HPV.
- Age: Common warts are seen primarily in children, while genital warts are most common in adolescents and young adults.
- Weakened immune system: Weakened immune systems put people at greater risk of HPV infections. HIV/AIDS or immune system-suppressing drugs used after organ transplants could lead to weakened immune systems.
- Damaged skin: If a person has open wounds around the skin, the risk of developing common warts will be higher.
- Personal contact: The risk of HPV infection also increases if a person touches someone’s warts or does not wear protection before coming into contact with surfaces exposed to HPV in places including swimming pools and public showers.
What are the tests to diagnose HPV?
Genital warts can be typically diagnosed by visual examination. However, high-risk forms of HPV don’t cause symptoms. This means you’ll likely learn about an infection through a routine screening.
- Pap Smear: Screens for cervical cancer and precancerous cells that may become cancer (cervical dysplasia) if left untreated.
- HPV test: Detects the high-risk strains of the virus that may lead to cervical cancer if left untreated.
- Colposcopy: If your Pap smear shows signs of abnormal cells or if you tested positive for HPV, your doctor may order Colposcopy for a closer visual examination of the cervix and vaginal wall. During this procedure, a lighted instrument called a colposcope magnifies your cervix, bringing abnormal cells into view. Your doctor may remove the cells and have them tested in a lab for signs of precancer or cancer (biopsy).
HPV Prevention and Vaccination

- Get screened and tested regularly. Early detection of HPV and abnormal cells prevents cervical cancer. Singapore’s Ministry of Health (MOH) recommends
- All women aged 25 and above have had sex to take either a Pap test once every three years (for women 25 to 29 years or
- HPV (or HPV DNA) test once every five years (for women 30 years and above).
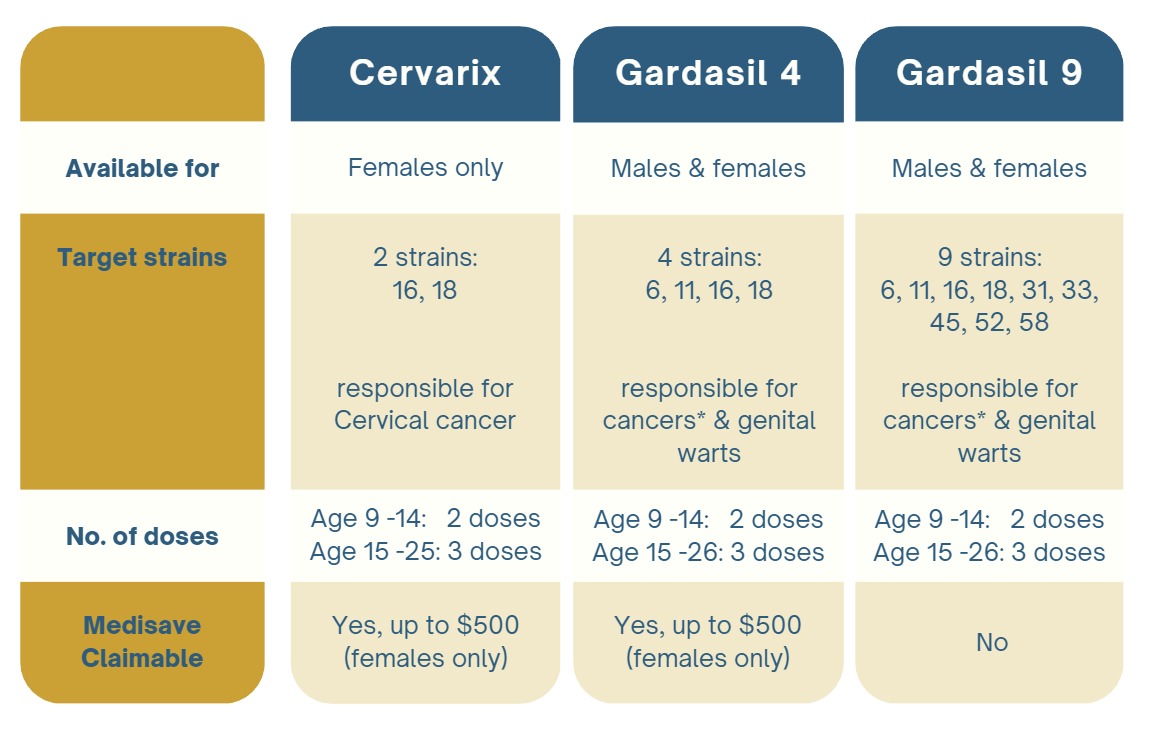
- Get HPV Vaccination. The best way to protect against HPV is to get vaccinated before becoming sexually active. There are a few options available in Singapore: Cervarix, Gardasil-4 and Gardasil-9.
- Practice safer sex. Condoms may be less effective at preventing HPV than protecting against STIs that spread through body fluids. However, using them correctly each time you have sex can reduce your risk of an HPV infection.
- Protect your partner(s). Share with your partners if you are diagnosed with HPV so they can get tested. You may need to stop having sex while you’re getting treated for genital warts or high-risk forms of HPV.
To reduce the risk of HPV infection, you can get vaccinated and undergo regular screening.
If you would like to get your vaccination or screening done, call Atlas Associates Clinic or WhatsApp us at 6956 6577.


